Breast cancer develops from cells in the breast. The most common sign of breast cancer is a new lump or mass, but most are benign.
Other signs include a generalized swelling of part of the breast (even if no lump is felt), skin irritation or dimpling, nipple pain or discharge, redness or scaliness of the nipple or breast skin, or a spontaneous discharge other than breast milk.
Provided here is key information on risk factors, prevention and detection of breast cancer.
Who is at risk?
Gender: Being a woman is the greatest risk factor for breast cancer. However, men can also develop breast cancer.
Age: The risk of developing breast cancer increases with age. Most invasive breast cancers are primarily found in women age 55 or older.
Heredity: Breast cancer risks are higher among women with a family history of the disease. Having a first-degree relative with breast cancer increases a woman’s risk. Having more than one first-degree relative who has or has had breast cancer before age 40 or in both breasts increases the risk even more.
However, most women with breast cancer don’t have a first-degree relative with the disease.
Other risk factors:
Post-menopausal hormone therapy with estrogen and progesterone therapy
Being overweight, especially excessive weight gain after menopause
More than one alcoholic drink daily
Physical inactivity
Long menstrual history
Never having children, or first live birth after age 30
Prevention
Some risk factors can’t be changed, such as age, race, family history and reproductive history. And while it’s not known how to prevent breast cancer, women of average risk can take steps to further reduce their risk. They include:
Reduce alcohol use
Breastfeed
Engage in regular physical activity
Maintain a healthy weight.
Detection
The earlier breast cancer is found, the better the chances for successful treatment. A mammogram often can show breast changes that may be cancer before physical symptoms develop. The American Cancer Society recommends the following guidelines for early detection:
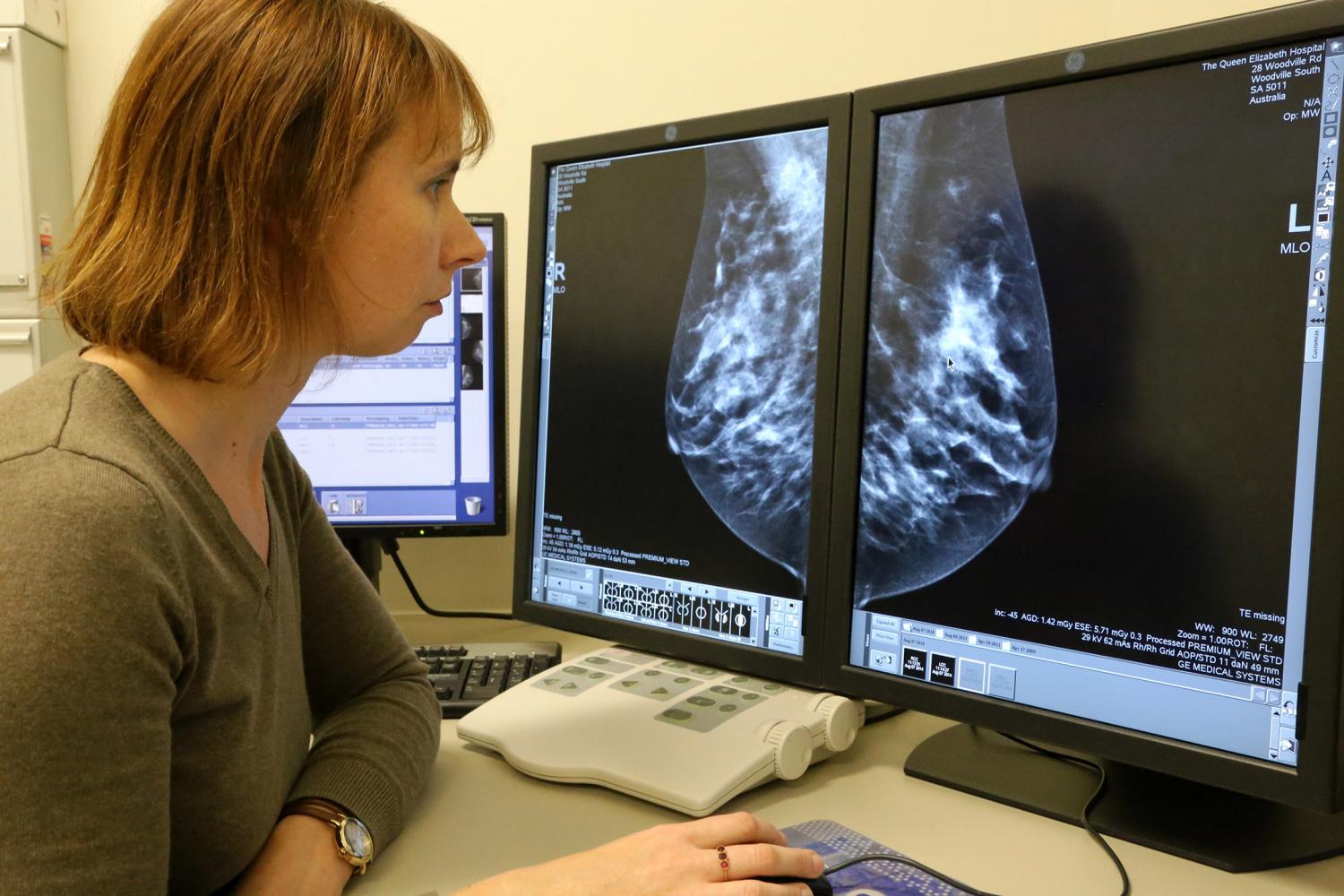
Women ages 40-44 should have the choice to start annual mammograms.
Women ages 45-54 should get mammograms every year.
Women 55 and older should switch to mammograms every two years, or can continue annual screening.
Screening should continue as long as a woman is in good health and expected to live 10 more years or longer.
All women should be familiar with the benefits, limitations and potential harms linked to breast cancer screening.
An MRI to screen for breast cancer is recommended for women at high risk, including women with a family history of breast or ovarian cancer. Also at high risk are women whose lifetime risk is 20 to 25 percent or greater based on family history, a known breast cancer gene mutation and women who were treated with radiation to the chest area when they were between the ages of 10 and 30.



Leave a Reply